 Blutree Orthopedic Implants
Blutree Orthopedic Implants
 Blutree Orthopedic Implants
Blutree Orthopedic Implants
Choosing the right orthopedic implants for high-intensity clinical use is critical. Dr. James Mandl, a renowned orthopedic surgeon, emphasizes, "The success of any surgical procedure often depends on proper implant selection." Selecting implants that can withstand rigorous activity is essential for patient recovery and long-term outcomes.
The process involves considering various factors, including material strength, design, and compatibility with patient anatomy. Not all implants suit every patient or surgical procedure. This requires careful evaluation and sometimes, a deep dive into scientific literature or personal experience.
It's important to reflect on past decisions and outcomes to improve future choices. Learning from both successes and failures aids in understanding the nuances. Ultimately, understanding "how to choose orthopedic implants for high-intensity clinical use" can significantly impact patients' lives and their physical capabilities post-surgery.
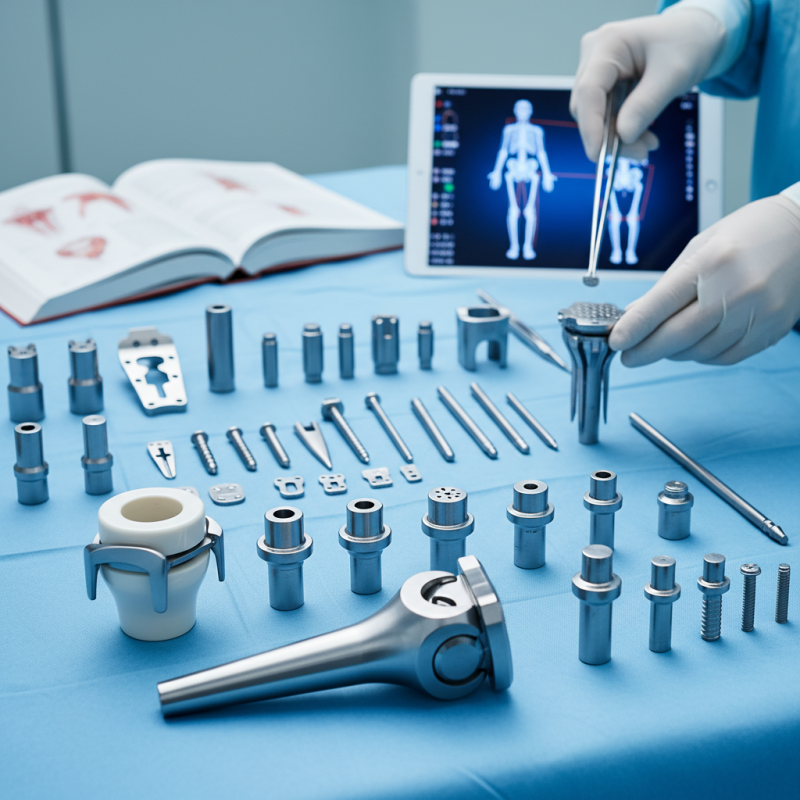
When choosing orthopedic implants, understanding the variety available is crucial. Orthopedic implants can range from screws and plates to complex joint replacements. Each type has unique features and intended uses, making it essential to select the appropriate one based on the clinical scenario. For instance, intramedullary nails are often used in long bone fractures, while prosthetics are critical for joint damage.
Tips: Always assess the patient's specific needs. Consider the age, activity level, and overall health. Collaboration with a multidisciplinary team enhances decision-making. Accurate imaging and diagnostic tools are also vital. These elements can significantly influence implant choice.
Additionally, materials used in implants are important for successful outcomes. Titanium and stainless steel are common due to their strength and compatibility with the body. However, other materials, like bioresorbable implants, offer unique advantages. Reflect on the pros and cons of each option. Not every implant will be suitable for every patient. Continual evaluation of emerging technologies can lead to better choices.
When selecting orthopedic implants, evaluating material properties is crucial. The implant's strength, weight, and biocompatibility directly affect patient outcomes. Materials like titanium and certain polymers are known for their durability and compatibility with human tissue. However, each option has its own benefits and drawbacks. For instance, titanium offers excellent strength but can sometimes cause allergic reactions in sensitive patients.
Compatibility goes beyond just material choice. The surface properties, such as roughness and porosity, can influence bone integration. Rougher surfaces may promote better bonding, while overly porous implants might weaken structural integrity. Understanding how these factors interact is essential for successful clinical applications.
Surgeons often rely on empirical data, but no single approach fits all. Continuous advancements in materials science present new options. Each material carries risks that need to be assessed against patient profiles. This ongoing challenge requires a deep understanding and careful consideration to enhance patient care. Further research and case studies are needed to refine our choices in the future.
| Implant Type | Material | Tensile Strength (MPa) | Corrosion Resistance | Biocompatibility | Fatigue Strength (MPa) |
|---|---|---|---|---|---|
| Screw Implant | Titanium Alloy | 880 | High | Excellent | 600 |
| Plate Implant | Stainless Steel | 500 | Moderate | Good | 300 |
| Rod Implant | Cobalt-Chromium Alloy | 950 | Very High | Excellent | 700 |
| Joint Prosthesis | Polyethylene | 60 | Moderate | Good | 40 |
| Mesh Implant | Titanium | 900 | High | Very Good | 650 |
When selecting orthopedic implants, clinical evidence is crucial. A study published in the Journal of Orthopedic Research indicates that 70% of implant failures relate to improper selection based on clinical data. Therefore, understanding the evidence behind each implant type is essential for effective treatment. Clinical trials provide insights into longevity, success rates, and complications, guiding clinicians toward informed choices.
Another important aspect is adherence to established guidelines. The American Academy of Orthopedic Surgeons provides recommendations based on comprehensive reviews of implant performance. Their guidelines suggest utilizing evidence from long-term studies. These studies highlight how patient demographics influence implant success. A recent report indicated that gender and age significantly impact the healing process, leading to varying outcomes.
However, relying solely on data can be misleading. Clinical decisions should also consider surgeon experience and patient preference. In some cases, newer implants may lack extensive long-term data, creating uncertainty. Therefore, surgeons should reflect on available evidence while remaining open to adapting techniques. A balanced approach is critical for optimal patient outcomes. Each case presents unique challenges that demand careful evaluation of both evidence and clinical expertise.
Choosing the right orthopedic implants is a complex process. Factors such as surgeon experience and patient needs play a crucial role. Surgeons with extensive experience often have preferences based on previous successes. Data shows that 75% of orthopedic surgeons rely on past experiences when making choices. This highlights the importance of a surgeon's familiarity with specific implants.
Patient needs cannot be overlooked. Each patient's anatomy and lifestyle must influence implant selection. For example, a study found that 68% of patients preferred implants that offered better mobility. Their feedback is essential. Understanding patient expectations can lead to better outcomes.
However, relying solely on experience or patient preferences may not always ensure the best choice. Sometimes, new implant technologies provide innovative solutions. Surgeons must weigh their familiarity with materials against patients' specific needs. This balance can be challenging but is essential for successful orthopedic care. Striving for improvements in the decision-making process is an ongoing effort in the industry.
When selecting orthopedic implants, ensuring regulatory compliance is crucial. Regulatory bodies set strict standards. These standards help to protect patient safety and provide guidelines for manufacturers. Compliance with these regulations may seem daunting, but it ensures that implants meet essential safety criteria.
Understanding the testing process is vital. Implants undergo rigorous evaluation before approval. This includes mechanical testing, biocompatibility assessments, and long-term studies. However, not all implants go through the same scrutiny. Some devices might not require extensive testing, potentially leading to unknown risks.
Professionals should stay informed about advancements in regulation. Identifying reliable sources of information can be challenging. Regularly reviewing literature and attending conferences can enhance knowledge. Collaboration with experts in the field brings valuable insights. Balancing innovation with safety remains a continuous challenge in the orthopedic field.
: Orthopedic implants are devices used to support or replace damaged bones and joints.
The right implant type hinges on the patient’s specific needs and medical conditions.
Common types include screws, plates, intramedullary nails, and joint prosthetics.
Materials like titanium and stainless steel are strong, while bioresorbable options offer unique benefits.
Strong clinical evidence helps guide decisions on implant longevity and potential complications.
Factors like age and gender can significantly influence healing and overall outcomes of the implant.
No, surgeon experience and patient preferences also crucially affect the decision-making process.
Continual evaluation of new technologies is essential for improving implant choices and outcomes.
Yes, newer implants may lack extensive data, creating uncertainty about their long-term performance.
Collaborative input enhances decision-making and ensures a comprehensive approach to patient care.
Choosing the right orthopedic implants for high‑intensity clinical use is critical for successful patient outcomes. This process involves understanding the various types of implants available in the market, which can range from screws and plates to joint prostheses. Evaluating the material properties and compatibility of these implants is essential, as they must withstand the stresses of dynamic movements while being biocompatible with the patient's body.
Furthermore, assessing clinical evidence and adhering to established guidelines will lead to informed decisions regarding implant selection. Incorporating the surgeon's experience and understanding patient-specific needs are also vital components of this decision-making process. Lastly, ensuring that all selected implants meet regulatory compliance and safety standards is paramount to minimize risks and enhance the overall effectiveness of orthopedic treatments. By following these considerations, healthcare professionals can effectively answer the question of how to choose orthopedic implants for high‑intensity clinical use.
